“I wasn’t expecting to feel full after two bites. That had never happened to me in 45 years.” — a real patient experience echoed by millions of people now taking GLP-1 medications worldwide.
If you’ve heard the word Ozempic everywhere lately — from your doctor’s office to celebrity gossip — you’re not imagining it. These medications have completely reshaped how we think about weight, diabetes, and metabolic health. And in 2026, they’re more widely used than ever before. This is your comprehensive Ozempic Guide 2026.
But what exactly is going on inside your body when you take one? Are they safe? Who really benefits? And what happens when you stop? This guide answers all of it — clearly, honestly, and without the hype.
1 in 5U.S. adults have now used a GLP-1 drug
15–20%Average body weight lost in clinical trials
10+FDA-approved GLP-1 drugs currently available
1. What Are GLP-1 Medications?
GLP-1 stands for Glucagon-Like Peptide-1. That sounds technical, but it’s actually a hormone your body already makes naturally — every time you eat.
When food enters your gut, your small intestine releases GLP-1. This hormone tells your pancreas to produce insulin, tells your brain you’re getting full, and slows down how quickly your stomach empties. It’s basically your body’s natural “I’ve had enough” signal.
The problem? In many people — especially those with type 2 diabetes or obesity — this signal is too weak, too short-lived, or gets ignored. GLP-1 receptor agonist medications mimic and amplify this hormone artificially, sending a stronger, longer-lasting version of that same signal.
✅ Key GLP-1 Medications Available (2026)
- Semaglutide injection → Ozempic (diabetes), Wegovy (weight loss)
- Semaglutide pill → Rybelsus (daily tablet, FDA approved 2019) + new Ozempic pill (2026)
- Tirzepatide → Mounjaro (diabetes), Zepbound (weight loss)
- Liraglutide → Victoza (diabetes), Saxenda (weight loss)
- Dulaglutide → Trulicity
2. What Is Ozempic Exactly?
For more detailed information and tips, check out our Ozempic Guide 2026.
Ozempic is the brand name for semaglutide, made by the Danish pharmaceutical company Novo Nordisk. It was originally approved by the FDA in 2017 specifically to treat type 2 diabetes in adults.
Since then, its reach has exploded. The same active ingredient (at a higher dose) powers Wegovy, which is FDA-approved specifically for weight loss.Combine medication with exercise routines (see latest Fitness and Body Trends). And in February 2026, the FDA approved a brand new Ozempic pill — a daily tablet version — expanding access even further for people who want to avoid injections.
Here’s the important thing most people miss: Ozempic is not technically a weight loss drug. It’s a diabetes medication. But because it causes significant weight loss as a side effect, it’s widely prescribed off-label for obesity — and Wegovy is the officially approved weight-loss version of the same molecule.Focus on high-protein foods and balanced meals (learn more in our Nutrition Guide)
3. How Does It Actually Work Inside Your Body?
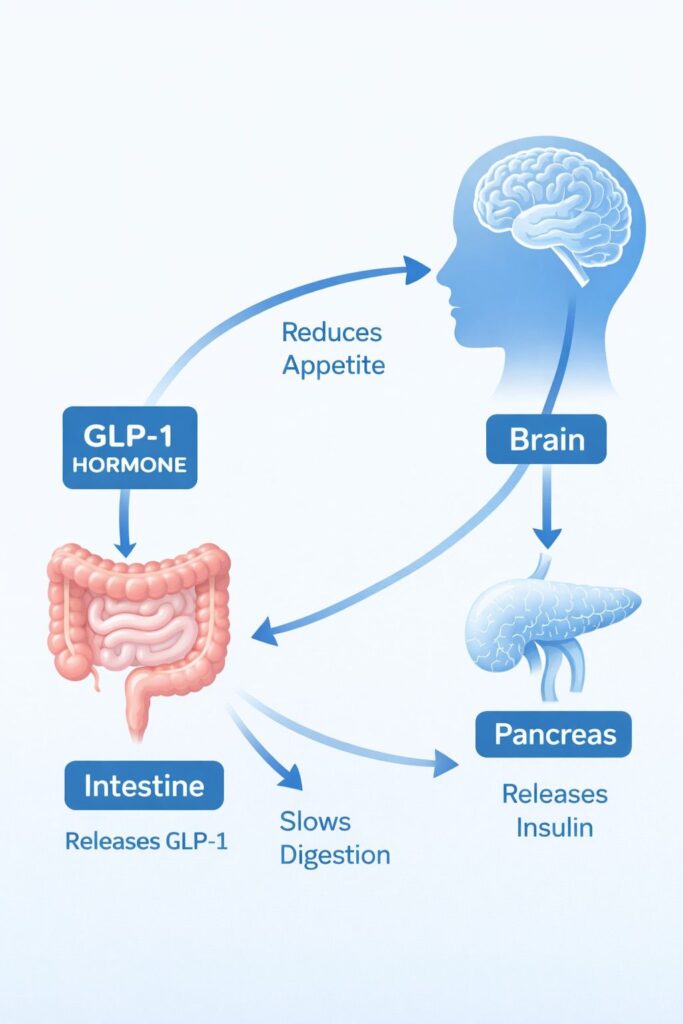
Think of semaglutide as a very convincing impersonator of your GLP-1 hormone — except it sticks around for about a week instead of a few minutes. Here’s what it actually does:
In Your Pancreas
When your blood sugar rises after eating, Ozempic triggers your pancreas to release insulin — the hormone that moves glucose out of your blood and into your cells for energy. Crucially, it only does this when blood sugar is already high. This makes it much safer than plain insulin injections, which can cause dangerous blood sugar crashes.
In Your Brain
GLP-1 receptors exist in the brain too — specifically in the areas that control hunger and reward. Semaglutide acts on these regions to reduce your appetite and diminish the pleasure response to food. That’s why people on Ozempic often report that they just… don’t think about food as much. The constant background noise of hunger gets quieter.Managing stress is also important for overall health (read our Exam Stress Management guide).
In Your Stomach
Ozempic slows down how fast your stomach empties after a meal. Food stays in your stomach longer, which means you feel full for longer. A meal that might have left you hungry two hours later now keeps you satisfied for four or five hours.
“It’s not willpower in a needle. It’s your body finally getting a signal it was too weak to hear before.”
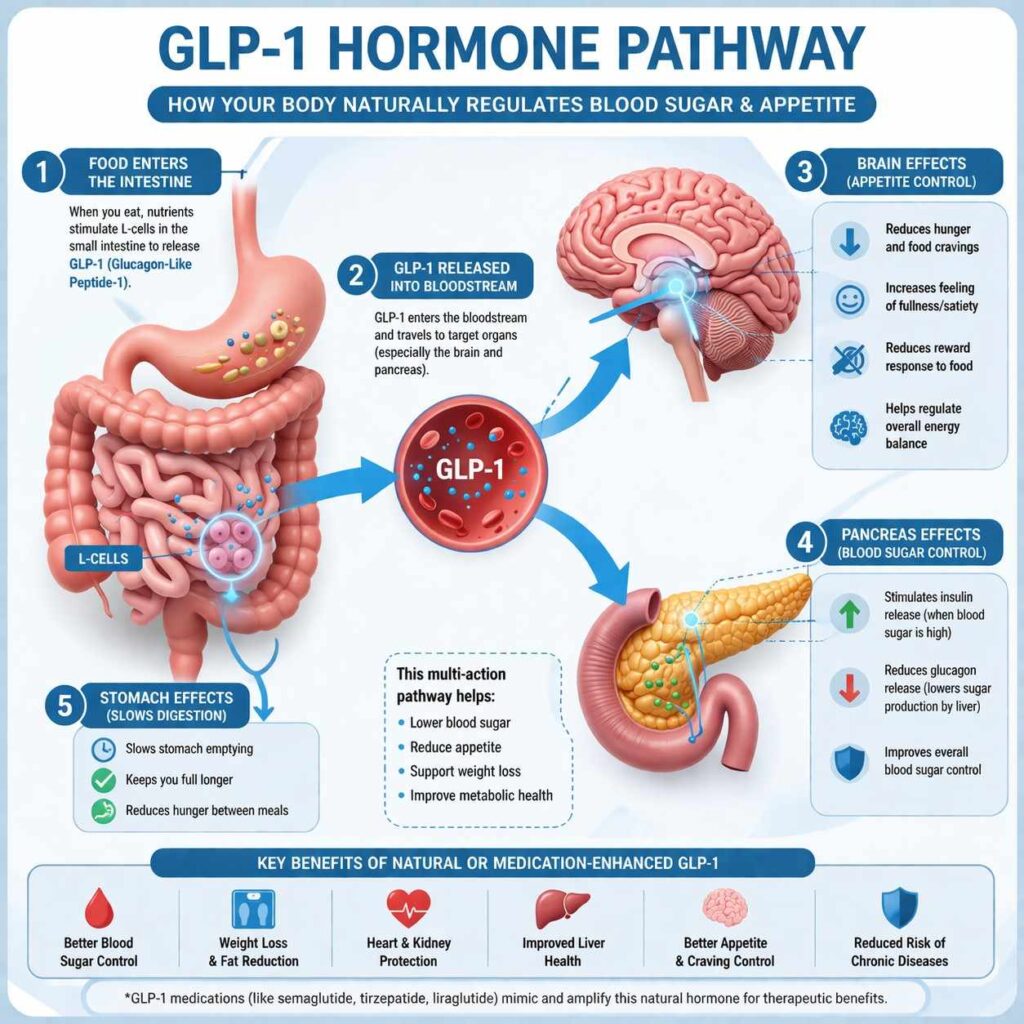
4. The Real Benefits — Way Beyond Just Weight Loss
Most people hear “Ozempic” and think “weight loss drug.” But the research over the past several years has revealed a surprisingly wide range of benefits:
🫀 Heart Protection
This is arguably the most important benefit outside of weight loss. Large clinical trials have shown that GLP-1 medications significantly reduce the risk of heart attack, stroke, and cardiovascular death in people with type 2 diabetes and existing heart disease. This is why Ozempic is FDA-approved not just for blood sugar control, but explicitly for cardiovascular risk reduction.
🫘 Kidney Disease Slowdown
A 2024 clinical trial (the FLOW trial) found that semaglutide slows the progression of chronic kidney disease in people with type 2 diabetes — reducing kidney failure risk and cardiovascular death. This was significant enough to earn Ozempic a new FDA approval specifically for kidney protection in 2026.
🧠 Brain & Mental Health
Emerging research is exploring GLP-1’s effects on the brain. Early studies suggest potential benefits for addiction behaviors (alcohol, opioids, and even compulsive eating), and researchers are investigating possible connections to reduced Alzheimer’s risk. This science is still early, but the signals are genuinely exciting.
🫁 Fatty Liver Disease
Semaglutide has received FDA approval for treating MASH (Metabolic Dysfunction-Associated Steatohepatitis) — a serious form of fatty liver disease. This is a major new frontier for GLP-1 medications.
⚖️ Significant, Sustained Weight Loss
People using GLP-1s for obesity have lost an average of 10–15% of body weight in clinical trials. The most powerful versions (like high-dose tirzepatide) have produced losses of over 20% — approaching what’s typically seen with bariatric surgery, without going under the knife.
✅ Additional Documented Benefits
- Lowered blood pressure
- Improved cholesterol and triglyceride levels
- Reduced inflammation markers
- Better sleep (often linked to reduced sleep apnea from weight loss)
- Improved PCOS symptoms in women
- Reduced arthritis symptoms (via weight reduction)
5. Side Effects You Absolutely Need to Know

Ozempic is not a free lunch. It comes with real side effects — most manageable, some serious. Ozempic may cause inflammation of the pancreas (pancreatitis).
Common Side Effects (Affect Most People)
⚠️ Most Common — Usually Temporary
- Nausea — The most reported side effect, especially in the first few weeks. Often improves as your body adjusts.
- Vomiting — Less common but possible, especially if you eat too quickly or too much.
- Diarrhea or constipation — Digestive system changes are very common early on.
- Stomach pain or bloating — Slowed digestion can cause discomfort.
- “Ozempic face” — Rapid fat loss can cause facial skin to look looser or more aged. This is actually a consequence of fast weight loss in general, not specific to semaglutide.
Doctors minimize these effects by starting at the lowest dose and gradually increasing over several months. Eating smaller, more frequent meals and avoiding strong smells can also help manage nausea.Some users report mood changes or emotional shifts, which can be linked to underlying mental illness.
Serious Side Effects (Less Common but Important)
🚨 Stop and Call Your Doctor Immediately If You Have:
- Severe stomach pain that radiates to your back — Could indicate pancreatitis (pancreas inflammation)
- Swelling or lump in your neck, trouble swallowing, or hoarseness — Possible thyroid tumor warning signs
- Sudden vision changes — Especially if you already have diabetic eye disease
- Signs of very low blood sugar — Shakiness, sweating, confusion (more likely if also taking insulin)
- Severe gallbladder symptoms — Right-side abdominal pain, nausea, fever
One note if you’re planning surgery: Ozempic slows stomach emptying, which can be dangerous under general anesthesia. Always tell your surgeon you’re taking it — you’ll likely need to stop it days before any procedure.For other serious health conditions, read about diseases like Meningitis.
Who should not take GLP-1 drugs:
- Anyone with a personal or family history of medullary thyroid cancer
- People with Multiple Endocrine Neoplasia syndrome type 2
- Those with a history of pancreatitis
- People with gastroparesis (already slow stomach emptying)
- Pregnant women or those planning pregnancy (stop at least 2 months before)
6. Ozempic vs Wegovy vs Mounjaro — What’s the Real Difference?
| Drug | Active Ingredient | FDA Approved For | How Often | Avg Weight Loss |
|---|---|---|---|---|
| Ozempic | Semaglutide | Type 2 Diabetes + Heart / Kidney protection | Weekly injection or daily pill (2026) | ~10–12% |
| Wegovy | Semaglutide (higher dose) | Chronic weight management | Weekly injection | ~15% |
| Mounjaro / Zepbound | Tirzepatide (GLP-1 + GIP dual agonist) | Diabetes (Mounjaro) / Weight loss (Zepbound) | Weekly injection | ~20–22% |
| Rybelsus | Semaglutide (oral) | Type 2 Diabetes | Daily pill | ~8–10% |
The short answer: Mounjaro/Zepbound produces more weight loss because it targets two hormones (GLP-1 and GIP) instead of one. But Ozempic/Wegovy has more long-term safety data and proven cardiovascular benefits. Your doctor should help you choose based on your specific situation.
7. Who Should Actually Consider GLP-1 Medications?
GLP-1 drugs are not for everyone who wants to lose 10 pounds before summer. They’re prescription medications with real risks, real costs, and real long-term commitments. Here’s who genuinely benefits:
✅ Good Candidates
- Adults with type 2 diabetes who need better blood sugar control
- Adults with a BMI of 30+ (obesity)
- Adults with BMI 27+ plus at least one weight-related health condition (high blood pressure, sleep apnea, high cholesterol, heart disease)
- People with diabetes who also have heart disease or kidney disease
- People who have tried lifestyle changes without achieving enough improvement
Most insurance plans in the US now cover GLP-1 drugs for diabetes, but coverage for weight loss alone varies widely. Costs can range from $900–$1,500/month without insurance — though prices have been steadily dropping as generic versions come to market.
8. The New Ozempic Pill — A 2026 Game Changer

For millions of people who are uncomfortable with weekly injections, 2026 brought a major development: Ozempic was FDA-approved as a daily oral tablet on February 4, 2026, available in three strengths (1.5mg, 4mg, and 9mg).
This is different from Rybelsus (the existing semaglutide pill), which uses a different formulation and dosing. The new Ozempic pill opens the door for people who’ve been hesitant about injections to access the same medication.
There is a catch: like Rybelsus, it requires strict timing — taken on an empty stomach with minimal water, at least 30 minutes before eating. People who find that routine difficult may still prefer the weekly injection for its simplicity.
9. What Happens When You Stop Taking It?
This is the question nobody likes to hear the answer to — but it’s critically important.
Clinical trials have shown that after stopping GLP-1 medications, most people regain about two-thirds of the weight they lost within one year. The reason is biological, not a lack of willpower. Once the drug leaves your system, hunger returns, cravings come back, and your stomach empties at its normal speed again.
This is why most endocrinologists now consider GLP-1 therapy a long-term — possibly lifelong — intervention for many patients, similar to how we treat high blood pressure with ongoing medication. It doesn’t fix the underlying cause; it manages the condition continuously.
⚠️ Practical Tips to Sustain Results
- Use the time on GLP-1 drugs to build sustainable eating habits and exercise routines
- Focus on high-protein foods to prevent muscle mass loss during weight loss
- Drink at least 2 liters of water daily — dehydration worsens side effects
- Work with a doctor to determine the right long-term plan for your specific situation
- Don’t stop abruptly without medical guidance
10. Frequently Asked Questions
Can I use Ozempic if I don’t have diabetes?
Yes, but through Wegovy — the weight-loss version of the same drug. Ozempic itself is technically approved only for type 2 diabetes, but doctors often prescribe it off-label for weight loss. Wegovy is the officially approved option for obesity without diabetes. Always consult your doctor about which is appropriate.
How long before I see results from Ozempic?
Most people notice reduced appetite within the first week or two. Visible weight loss typically begins within 4–8 weeks, but significant results (5–10% body weight) usually appear at the 3–6 month mark. Blood sugar improvements in diabetics can begin within days of the first dose.
Is Ozempic safe for long-term use?
GLP-1 drugs have been used for type 2 diabetes for over 20 years. Long-term studies show they are generally safe for most people. Regular check-ins with your doctor are important to monitor kidney function, pancreas health, and other markers. No drug is without risk, but the long-term safety profile is considered strong for appropriate candidates.
Can I drink alcohol while on Ozempic?
Alcohol can increase the risk of low blood sugar when combined with GLP-1 drugs, especially if you’re also on other diabetes medications. Many people find their tolerance for alcohol decreases significantly on Ozempic. It’s not strictly forbidden, but drink minimally and always discuss with your doctor.
What is “Ozempic face” and should I be worried?
“Ozempic face” refers to facial skin that looks looser, more gaunt, or more aged after rapid weight loss. It’s not unique to Ozempic — any rapid weight loss can cause this. Slower, more gradual weight loss tends to minimize this effect. It can be managed cosmetically if it’s a significant concern, and some people find it improves over time as skin adjusts.
Is Mounjaro better than Ozempic?
Mounjaro (tirzepatide) tends to produce greater weight loss than Ozempic (semaglutide) — often 20%+ vs 12–15%. This is because tirzepatide targets two hormones (GLP-1 and GIP) while semaglutide targets one. However, Ozempic has more established long-term cardiovascular safety data. The “better” drug depends entirely on your individual health profile, goals, and what your doctor recommends.
Conclusion
GLP-1 medications like Ozempic have genuinely earned their place at the center of modern health conversations. They’re not miracle drugs — but for the right people, they’re close to it. The combination of blood sugar control, meaningful weight loss, and documented heart and kidney protection makes them one of the most significant medical advances in metabolic health in decades.
That said, they are serious medications with real side effects, real costs, and a real question about long-term dependence. The decision to start, continue, or stop should always be made with your doctor — not based on celebrity endorsements or social media trends.
If you’re curious whether GLP-1 medications might be right for you, start with a conversation with your healthcare provider. Bring this guide along. Ask the hard questions. Your health deserves that level of attention.
⚕️ Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a licensed healthcare provider before starting, stopping, or changing any medication. Individual results and suitability vary. The information in this article is based on research current as of April 2026.

